Psilocybin is the bioactive component of a series of hallucinogenic fungi colloquially referred to as “magic mushrooms.” It is a naturally occurring psychedelic agent that has profound effects on behavior, cognition, and perception in large doses, and has historically been used for the religious and spiritual ceremonies of numerous indigenous communities.[1]
More recently, it has been associated with the “hippie” counterculture movement of the 1960s and 70s. During this time, Psilocybin mushrooms earned a relatively negative public stigma because of their mind-altering and reality-distorting potential, and in the 1970s, many global governments discouraged or outright banned scientific research into naturally occurring psychedelics. However, in recent years, there has been some clinical attention redirected towards the study of Psilocybin as a therapeutic agent for various ailments, particularly neuropsychiatric and substance abuse disorders.[2] This is partially because, of all psychedelic drugs, Psilocybin is reported to have the most favorable safety profile, with the potential to meet the therapeutic needs for a number of physiological ailments without the addictiveness and overdose risk of other mind-altering substances.
Recently, Psilocybin mushrooms have been clinically evaluated for their antidepressant and anxiolytic properties in particular, and the results appear to be very promising. In the correct dosage and in the proper environment, Psilocybin therapy has become somewhat popularized for treating a wide variety of other indications as well, from alcohol abuse to chronic pain. Furthermore, there has been a public boom in “microdosing” Psilocybin mushrooms in recent years, which refers to the process of consuming sub-hallucinogenic dosages of so-called magic mushrooms in order to manage stress, anxiety, or depression, clarify cognition, stimulate creativity, and regulate one’s mood. While there have been very limited clinical studies to date regarding the long-term effects of microdosing, many physicians recognize a social need for these studies amidst what is being described as a “Psychedelic Renaissance.”[3]
Benefits
Anxiety
Psilocybin has gained some widespread recent attention in news media for its anxiolytic potential. This might seem surprising, given that so-called magic mushrooms are alternatively known for their potential to cause hallucinations and, potentially, paranoia and other discomfiting symptoms under certain circumstances. Indeed, though moderate-to-large doses of Psilocybin are known to induce potentially distressing effects associated with psychedelia in certain circumstances, in smaller doses the hallucinogenic compound found in these mushrooms may actually yield long-term benefits when it comes to alleviating anxiety. And these observations do not simply stem from anecdotes; they are backed by peer-reviewed publications of double-blind clinical trials.
A 2020 study published by Psychiatry Research conducted a meta-analysis of the experimental effects of Psilocybin on patients with anxiety and depression. The peer-reviewed publication evaluated four total studies, one of which was uncontrolled and three of which were randomized and placebo-controlled in a laboratory environment. Across the three controlled studies, researchers noted that anxiolytic effects were large and statistically significant. Further, no seriously adverse effects were reported among patients who microdosed. The researchers “tentatively” stated that they would recommend future research on Psilocybin for chronically anxious patients. [4]
Another noteworthy study was conducted in 2016, by the British Association for Psychopharmacology. Researchers evaluated the effects of single-dose Psilocybin and, alternatively, niacin on 29 patients with cancer-related anxiety and depression, in conjunction with psychotherapy. The study was placebo-controlled and double-blind. Outcomes indicated that Psilocybin “produced immediate, substantial, and sustained improvement in anxiety and depression and led to decreases in cancer-related demoralization and hopelessness, improved spiritual well-being, and increased quality of life.” Further, at the 6.5-month follow up, Psilocybin was associated with long-term anxiolytic and anti-depressant effects in roughly 60-80% of patients.[5]
This last example comes from a non-laboratory study; however, it bears relevance and legitimacy as it was peer-reviewed and conducted by psychopharmacologists, so it may be of interest regardless. In a 2019 study published by Frontiers in Psychiatry, researchers collected online questionnaire responses from 410 people from various countries. These participants offered evidence for psychiatric health ailments, plus past experience with psychedelics, most commonly Psilocybin. Unsurprisingly, the researchers found that individuals with anxiety found micro-doses of Psilocybin to be less immediately effective than full doses of the substance; however, they also noted that they felt that microdoses of Psilocybin were actually more effective long-term in comparison to their prescription medications.
It appears that Psilocybin possesses promising potential as an anxiolytic therapeutic, particularly for patients for whom other medical interventions have been ineffective. With this all being said, psychiatrists generally urge those interested in microdosing Psilocybin to exercise caution. There are very few placebo-controlled, double-blind studies associated with Psilocybin’s anxiolytic potential other than the ones mentioned above, and this limits physicians’ ability to provide a thoroughly informed recommendation for therapeutic use. Psychiatrists Joseph M. Barnby and Mitul A. Mehta of the Institute of Psychiatry, Psychology & Neuroscience at King’s College London, for example, advise that, though “psychedelic science…continues to grow and progress forward” in promising ways, patients are advised to be careful with these powerful compounds and avoid “losing control” due to overuse.[6]
Depression
Psilocybin has demonstrated potential in some peer-reviewed studies to exhibit antidepressant potential alongside its anxiolytic properties. In particular, Psilocybin has emerged as a possible therapeutic compound of interest for individuals who have treatment-resistant depression. In 2016, the LANCET Journal of Psychiatry conducted an open-label feasibility trial in which 12 patients with moderate-to-severe treatment-resistant depression received two oral doses of Psilocybin (10 mg and 25 mg, 7 days apart) in a supportive, controlled setting. Some patients exhibited transient anxiety or mild nausea after ingestion, but researchers reported that these symptoms became negligible around 6 hours after dosing. Relative to baseline, they found that depressive symptoms were reduced 1 week and 3 months after high-dose treatment. They also noted sustained improvements in anxiety. However, it is worth noting in this trial that there was no control group for this particular trial, which is generally inadvisable in clinical research.[7]
A more recent 2021 trial evaluated the efficacy of Psilocybin versus the Selective Serotonin Reuptake Inhibitor (SSRI) Escitalopram for major depression in a double-blind, randomized, controlled trial involving patients with long-term, moderate-to-severe depressive disorder. A total of 59 patients underwent this trial over 6 weeks. On the basis of the change in depression scores at week 6, the trial did not indicate a significant difference in antidepressant effects between Psilocybin and Escitalopram. The researchers suggested that larger and longer trials should be conducted to get a better idea of Psilocybin’s efficacy in relationship to other established major depression medications. [8]
On the other hand, if we look back to the study published in 2016 by the British Association of Pharmacology (refer back to Anxiety section), patients with cancer-related anxiety and depression appeared to show a marked improvement in terms of psychiatric distress as a result of minimal Psilocybin administration.
A 2015 study published by the Journal of Psychopharmacology pointed out that any classic psychedelic substance – including Psilocybin but also including ayahuasca, mescaline, or peyote, among others – was associated with reduced likely hood of psychological distress and, more specifically, suicidal thinking and attempts over the course of the next month to a year after use. This study was one of the first to indicate that psychedelics might be tentatively advisable in the treatment of mental health issues among adults.
Also in 2015, the scholars who published this study conducted a follow-up safety evaluation of the potential risk profile of therapeutic applications of Psilocybin in particular. They evaluated suicidality and mental health concerns among individuals who took Psilocybin in conjunction with other psychedelics, individuals who took non-Psilocybin psychedelics only, and a no-psychedelic control group. Results indicated that the outcomes of suicidal distress, suicidal thinking, and suicidal planning were categorically reduced in a statistically significant way for the group that used Psilocybin only. The odds of suicidal distress, thinking, and planning were reduced marginally less in the group that used Psilocybin in conjunction with other psychedelics, indicating that Psilocybin may possibly have the greatest therapeutic potential among several classes of psychedelics.[9]
PTSD
According to researchers, psychedelics like Psilocybin are “shaking up psychiatry,” and are forcing regulators to consider ways to safely administer these powerful substances to individuals who need treatment for PTSD, or Post-Traumatic Stress Disorder. PTSD, which is defined as a mental health condition triggered by a traumatic event or series of events that results in flashbacks, nightmares, chronic anxiety, depression, and uncontrollable, obsessive thoughts about the event, is challenging to treat due to its high rates of psychiatric and medical comorbidity. According to Bostoen et al, the “search for and development of drugs with new mechanisms of action [in the treatment of PTSD] has stalled.” However, within the past two years, two psychedelics have received “breakthrough designations” as possible therapeutics for psychiatric illnesses such as PTSD from the US Food and Drug Administration. One of these was Psilocybin, and the other was 3,4-Methylenedioxymethamphetamine, or MDMA.
Before PTSD was introduced as a psychiatric diagnosis in the third edition of the Diagnostic and Statistical Manual of Mental Disorders in 1980, LSD, Psilocybin, and Ketamine were sometimes used in the Netherlands as therapeutic tools for the treatment of what was then called “Concentration Camp Syndrome,” a specific type of PTSD. This therapy enabled clients to reexperience traumatic events under therapeutic guidance, and many were treated with classical psychedelics. However, it cannot be said for sure that there were any improvements specifically related to patients with PTSD, as this was not an official diagnosis at the time.[10]
In terms of contemporary research, there have not been any placebo-controlled studies evaluating Psilocybin’s effect on patients officially diagnosed with PTSD. Many researchers have explored the rationale behind using Psilocybin in the treatment for PTSD, such as one piece of literature published by the International Review of Psychiatry in 2021, in which researchers explored combined pharmacological and psychotherapeutic approaches in the treatment of PTSD and co-morbid Major Depression. They specifically focused on Psilocybin and MDMA, which, again, have been indicated as “breakthrough therapeutics” by the US Food and Drug Administration. However, more clinical research specifically related to PTSD must be conducted in order to evaluate these psychedelics’ true efficacy.[11]
Migraines
Recently, Psilocybin has demonstrated potential in the treatment of headache disorders, including chronic migraine. A small-scale study published by Neurotherapeutics in 2021 administered oral placebo and Psilocybin (0.143 mg/kg) to patients in two test sessions spaced two weeks apart, and had the subjects record headache diaries. Over the two-week period measured after single administration, the reduction in weekly migraine days from baseline was statistically greater after Psilocybin administration in comparison to the placebo group. Further, the researchers noted the Psilocybin was well-tolerated ta low doses; there were no unexpected or serious adverse effects of withdrawals. They recommended further research regarding Psilocybin’s therapeutic effects for migraine sufferers.[12]
OCD
In a study published by the Journal of Psychoactive Drugs in 2021, researchers observed the long-term amelioration of OCD symptoms in a patient via the consumption of Psilocybin-containing mushrooms. They presented the case of a male adult with OCD who demonstrated clinically and statistically meaningful reduction of his symptomatology after long-term consumption of Psilocybin. With that being said, this study only evaluated a single patient, and much more robust, long-term, multi-patient studies should be required before any firm conclusions are drawn related to Psilocybin’s efficacy as an OCD therapeutic specifically.[13]
With that being said, there is some promise that more robust studies will be conducted soon. For example, a study by Yale University, which will involve 30 participants with OCD receiving a single high dose of Psilocybin, is expected to be completed by early 2022.[14]
ADHD
To date, no official clinical studies have been published evaluating Psilocybin’s efficacy as a therapeutic for individuals with Attention Deficit Hyperactive Disorder (ADHD). However, there are certainly implications that the hallucinogenic substance’s mechanisms in the brain might be efficacious in the treatment of attentional deficits in individuals with conditions like autism and ADHD. Specifically, researchers (in this case, from the University of Queensland) observed that hallucinogenic doses of Psilocybin had an effect on “binocular rivalry rates,” which are linked to attention and arousal. In other words, Psilocybin slowed binocular rivalry switching in the brain through serotonin modulation, which may indicate the hallucinogenic as a beneficial treatment for individuals with attention issues.[15]
Bipolar
Bipolar Disorder bears a particularly precarious relationship with hallucinogenic substances, as psychedelic abuse has actually been linked to the development of psychiatric illnesses such as schizophrenia and Bipolar Disorder. For example, in a case study published in 2021, a woman who ingested Psilocybin mushrooms reported an episode of mania when she had not previously been diagnosed with either Bipolar I or II.[16]
On the other hand, there is still some interest in the careful, controlled administration of Psilocybin to individuals who suffer from Bipolar Disorder due to its clinically significant potential to treat depression, which is also a Bipolar symptom. However, studies relating Psilocybin and Bipolar are presently still in the risk-evaluative phase, given the tenuous nature of the disorder. For example, a study published by The BMJ at Yale explored the risk of taking Psilocybin for the treatment of Bipolar Depression. Specifically, researchers presented a comprehensive list of case studies published through December 31, 2020 via PubMed, Web of Science, and PsychInfo concerning classical psychedelics in psychiatric clinical trials. Only 4 of 15 cases addressed Psilocybin and involved individuals with Bipolar Disorder. These studies indicated some risk of activating mania with Psilocybin in patients with Bipolar Depression, but that this risk is not apparently “strong or overwhelming” enough to discourage further research with careful controls.[17]
Epilepsy
There is a rather long history of interest regarding Psilocybin and other classical psychedelics in the treatment of epilepsy, dating back to the early 70s. For example, in a journal published by Electroencephalography and Clinical Neurophysiology in 1971 explored the effects of Psilocybin, Dimethyltryptamine, and Mescaline on photically induced epilepsy in the baboon (Papio papio). Results yielded that Psilocybin resembled LSD 25 in modifying transmission in the visual pathway response to flash stimulation, whereas Methysergide did not alter evoked responses in the visual cortex. Researchers suggested that a serotoninergic system is “probably involved” in the epileptic responses of the baboon to intermittent photic stimulation (ILS).[18] However, despite this long-term interest in psychedelics and epilepsy, there have been no clinical studies published to date evaluating Psilocybin and its potential therapeutic effects in human epileptic patients. As such, further studies are sorely needed in this regard.
Smoking Cessation
A noteworthy 2016 study published by The American Journal of Drug and Alcohol Abuse evaluated smoking cessation in Psilocybin-treated patients and followed up with them for 12 months. All 15 participants participated in the follow-up study, and 10 out of the Psilocybin-administered 15 remained smoking-abstinent. The researchers recommended further clinical study in terms of Psilocybin-facilitated treatment of substance use disorders.[19]
And indeed, more studies appear to be on the way. According to Neuroscience News and Research, Johns Hopkins University plants to evaluate the scientific mechanisms behind Mydecine’s purified Psilocybin drug MYCO-001 in relationship to smoking cessation in 2022. The study will take the form of a phase 2/3 clinical trial and will be placebo-controlled.[20]
Tinnitus
To date, there have been no clinical, placebo-controlled studies evaluating Psilocybin’s effect on tinnitus, which refers to a persistent and troublesome ringing sensation in the ears. In fact, a case report published by the Journal of Psychoactive Drugs demonstrated that a 39-year-old male actually developed tinnitus after inhaling N,N-dimethyltryptamine (DMT), and that the ear ringing was exacerbated after a microdose of Psilocybin mushrooms on two separate occasions. However, it is worth noting that this patient had a remote history of polysubstance use disorder.[21]
With that being said, there appears to be some theoretical interest regarding Psilocybin’s potential to treat tinnitus. On the online TinnitusTalk support forum, several users reported that their tinnitus abated or vanished entirely as a result of ingesting Psilocybin mushrooms.[22] However, this is all casual, anecdotal evidence and further research is necessary to evaluate whether Psilocybin has an ameliorating or exacerbating effect on tinnitus.
Alzheimer’s
According to Jones and Kelly, published in Frontiers in Synaptic Neuroscience, to date there are no disease-modifying treatments for Alzheimer’s Disease or any other dementia subtype. As a result of the “Psychedelic Renaissance” that has been occurring in the medical community over the last couple of years, however, there has been some interest involving Psilocybin and Lysergic Acid Diethylamide (LSD) in the treatment of Alzheimer’s dementia. Put simply, the theory is that, because psychedelics have potent anti-inflammatory properties that are overwhelmingly targeted toward brain tissue, they may represent a unique therapeutic pathway in the hippocampus.[23]
To date, there have not been any published clinical studies evaluating Psilocybin’s effect on memory, cognition, and dementia associated with Alzheimer’s. However, since 2019 there has been an ongoing study examining Psilocybin as a therapeutic in individuals with Mild Cognitive Impairment (MCI) or early Alzheimer’s Disease. Though conclusions have not been published, researchers have alluded to “encouraging results” thus far.[24]
Memory
According to researchers Barrett et al, published in NeuroImage, psychedelic drugs (including Psilocybin) modulate claustrum function in humans, with the claustrum being a subcortical nucleus that provides glutamatergic inputs to almost all areas of the cerebral cortex. In this study of 15 healthy participants, researchers found that Psilocybin’s activity in the claustrum impacts brain networks that support perception, memory, and attention. Researchers are still attempting to understand the exact mechanisms of psychedelics in the brain in relationship to memory, but these results are promising for patients with short-term or long-term memory impairments and perhaps attention deficit issues.[25]
On the other hand, it appears that high dosages of Psilocybin are actually associated with memory impairment as opposed to enhancement, whereas low doses produce no impairment. According to Healy with Psychopharmacology, low doses of classical psychedelics can increase the vividness of autobiographical memory and stimulate enhanced recall, often causing users to remember memories that had previously forgotten.[26]
Alcoholism
According to Meinhardt et al, published in Science Advances, Psilocybin targets a cognitive mechanism causing intellectual impairment and increased craving in individuals with alcoholism. In a 2021 study, these researchers demonstrated a causal link between pre-frontal mGluR2 function and impaired executive control, as well as alcohol craving. They found that restoring prefrontal mGluR2 levels in alcohol-dependent rats reduced these characteristics. These findings are promising for individuals struggling with alcoholism and may indicate the therapeutic capacity of Psilocybin in alcohol-dependent patients.[27]
A human study published by the British Association for Psychopharmacology yielded similar results. 10 volunteers with alcohol dependence received oral Psilocybin in one or two supervised sessions. Results demonstrated that, while abstinence did not increase significantly in the first four weeks of therapeutic treatment, it increased significantly following Psilocybin administration. Further, there were no treatment-associated adverse effects in participants. Researchers recommended further study regarding Psilocybin’s capacity as a therapeutic for alcohol dependence.[28]
Asperger Syndrome
Though there have been no human studies evaluating Psilocybin’s effect on the autistic brain (Autism Spectrum Disorder is sometimes referred to as Asperger Syndrome, depending on the individual’s functional placement on the autism spectrum), but there has been one 2020 study in an animal model of autism that explored Psilocybin as a therapeutic agent. Asperger Syndrome is characterized in part by difficulties in social interaction and nonverbal communication, and researchers explored whether Psilocybin had any impact on the sociability of rats with Autism Spectrum Disorder. According to findings, Psilocybin ameliorated the social behavioral abnormalities initially present in autistic mice. Further research is needed to evaluate Psilocybin’s impact on autistic individuals.[29]
Weight Loss & Appetite
Research regarding Psilocybin’s impact on obesity, weight management, eating disorders, and appetite is still in its infancy. However, there appear to be some interesting clinical studies on the horizon. Eating disorder specialist and epidemiologist Dr. C. Laird Birmingham has, in partnership with psychedelics research startup NeonMind, has started designing a study (as of 2021) that examines whether Psilocybin could be effective for weight loss purposes. The study will take place at the University of British Columbia and will examine the ways in which Psilocybin’s neural mechanisms can help the brain “stop linking life stress and trauma to eating behavior.”[30]
Fibromyalgia
California-based Tryp Therapeutics is partnering with scientists at the Chronic Pain & Fatigue Center at the University of Michigan for a study that will be the first of its kind, exploring the efficacy of Psilocybin in treating fibromyalgia. Specifically, the study will examine the safety and efficacy of TRYP-8802, a synthetic oral Psilocybin medication developed by Tryp Therapeutics. The study will commence on January 1, 2022 and will explore how TRYP-8802 may reorganize neural networks in the brain.[31] Hopefully, results will be positive for fibromyalgia sufferers, whose existing methods of treatment (usually non-steroidal anti-inflammatory drugs and gabapentinoids) are often characterized by unpleasant side effects and limited efficacy in terms of pain management.[32]
Chronic Pain
Psilocybin has not been well-studied in relationship to its therapeutic effects on chronic pain; however, there is some medical interest as well as anecdotal evidence that indicates that Psilocybin may be a promising drug in terms of pain management. In an article with Practical Pain Management, William Jones (a pseudonym), a chronic pain sufferer, describes his morning routine with Psilocybin: “Every day, William Jones puts some psilocybin mushrooms into a coffee grinder…and transfers them to gel capsules. He swallows the capsules with a sip of water, and within 20 to 30 minutes, he feels relief from the pain that has followed him since he was diagnosed with autoimmune peripheral neuropathy in 2005.” Of course, this is anecdotal and establishing a therapeutic relationship between Psilocybin and chronic pain requires robust clinical research. Fortunately, it appears that some is on the horizon. At the University of California in San Francisco, a study will examine whether Psilocybin therapy is effective for people with chronic lower back pain, staring in 2022.[33]
Meditation
There has been some clinical psychiatric attention focused on the confluence of mindfulness meditation and Psilocybin in the treatment of several psychological issues, from chronic depression to social anxiety. For example, at the University of Zurich, 38 adult meditators were selected to try Psilocybin-assisted therapy (versus placebo) for five days on a group meditation retreat. Four months later, they filled out a survey questioning them about changes in their attitudes, behavior, moods, and social experiences. Researchers reported that, in particular, these individuals reported less self-consciousness and better social functioning, even four months after the trial. It would appear, based on this study, that mindfulness meditation may enhance the positive effects of Psilocybin. Of course, more research is needed, but these results seem promising.[34]
Cluster Headaches
Cluster headaches constitute a rare and poorly understood disorder that causes extremely severe, debilitating head pain, specifically centralized around one eye. They occur in “clusters” that can continue for up to three to four months. These traumatic headaches have been described as “more painful than childbirth, gunshot wounds, and kidney stones,” earning them the ominous nickname “the suicide headache.” Patients are often desperate for effective treatment.[35]
A study published by Neurology evaluated 53 cluster headache patients who had used Psilocybin or LSD to treat their condition. 22 of 26 Psilocybin users reported that Psilocybin aborted the cluster attacks entirely; 25 of 48 reported cluster period amelioration; and 18 of 19 reported remission period extension. Researchers concluded that further research is warranted in this area.[36]
Serotonin
The psychedelic effects of Psilocybin are believed to emerge through the stimulation of serotonin 2A receptors (5-HT2ARs) via the active metabolite psilocin. In a study published by Neuropsychopharmacology, researchers evaluated the subjective intensity of psychedelic effects after a single oral intake o Psilocybin by subjecting volunteers to Positron Emission Tomography (PET) scans. Evidence pointed to the fact that Psilocybin intake leads to significant 5-HT2AR occupancy in the human brain, and that serotonin levels constitute key determinants in terms of the psychedelic experience.[37]
The interesting thing about this is that, though Psilocybin has demonstrated some potential efficacy in the treatment of depression, it actually does the opposite of what Selective Serotonin Reuptake Inhibitors (or SSRIs, which are common antidepressant medications) do in the brain. Rather than having an emotional blunting effect, Psilocybin appears to “increase emotional connection,” according to neuroscientist Leor Roseman of Imperial College London, rather than “reinforcing emotional avoidance and disconnection.” The implications of this are still being studied, but it is clear that serotonin levels play a pivotal role in Psilocybin’s effects on patients with mood disorders.[38]
Neurogenesis
In a study from Yale University, researchers demonstrated that a single dose of Psilocybin in a laboratory mouse model prompted a long-lasting increase in connections between neurons. This has implications, many researchers argue, for depressive patients, because chronic stress and depression are known to drastically reduce neuronal connections in the brain.[39]
Further, a 2021 study found that a dose of Psilocybin increases dendritic spine density within 24 hours of ingestion. An increase in spine density correlates to an increase in the number of excitatory synapses per neuron, which means more neuronal connections. More neuronal connections translate to better memory, increased capacity for learning, and less proclivity for depression and anxiety.[40]
Effects on the Brain
When one ingests Psilocybin, the gut converts it to its active metabolite, psilocin, which binds to serotonin 2A receptors. Researchers believe that this is what triggers “neuronal avalanching,” or essentially a domino effect of different changes in the brain’s many domains, from heightening activity in the visual cortex to decreasing activity in the default mode network, leading to what many describe as a ”loss of ego.” Further, Psilocybin increases connectivity among different regions of the brain, which ordinarily operate fairly independently, or in a compartmentalized fashion.[41]
Experience & Visuals
The experience of a Magic Mushroom trip depends on the dosage. In low doses, individuals report that colors are brighter, visuals look like they’re in high definition, and sound is enhanced. People who are sensitive to psychedelics might experience a change in perception on a dose as low as 0.5 grams of mushroom. With a medium dose (roughly 1-2.5 grams), individuals have reported visualizing notably vivid and enhanced colors, seeing geometric patterns overlaid on objects, which tend to move, morph, and “breathe,” and experiencing synesthesia, which occurs when perceptions overlap, so one can “hear colors” or “see sounds,” for example. A high dose (2.5-5 grams) can induce very vivid auditory and visual hallucinations that vary based on the individual. Some have described the visual experience of tripping on mushrooms as inducing “the colors and tones of a dream.”[42]
With a positive trip, an individual taking Psilocybin might experience tranquility, gratitude, empathy, euphoria, and, in some cases, feelings of intense spirituality or “sacredness.” With a negative trip, individuals might experience anxiety, fear, panic, and/or intense dread. Further, there is an increased chance of stomach upset and vomiting – as well as increases in heart rate, blood pressure, and temperature – in mid- to high-doses of Psilocybin. In high doses, individuals may also experience muscle weakness and a loss of coordination, which is why it is critical to have a safety buddy (sometimes called a “trip sitter”) nearby so that the individual ingesting Psilocybin does not jeopardize his/her own safety.
Whether the individual experiences a positive or negative trip depends on several factors, including one’s mood, expectations, beliefs, disposition, and personality, as well as the setting, individuals, and physical environment the individual is in when tripping.[43]
Typically, individuals experience hallucinations (mild or moderate) or at least visual distortions about an hour after mushroom ingestion.
Dosage
How to calculate your dose
The chemical content of magic mushrooms varies. Two randomly selected mushrooms can have different Psilocybin levels, for example, and laboratory testing is the only precise way to establish the potency of any given mushroom. Of course, there is currently no legal, regulated system for dosing magic mushrooms at the present time, so dosing guidelines are generally estimated by users based on some published clinical data on the Psilocybin content of these mushroom species, the most common being Psilocybe cubensis. For example, a low dose (1 gram) of magic mushrooms is likely to contain about 10 mg of Psilocybin, while a medium dose (1.75 grams, roughly) will correlate to 17.5 mg of Psilocybin, and a high dose (3.5 grams) will have roughly 35 mg.[44]
Dosage Levels
Microdosing involves taking roughly one-tenth of the “trip” dose of magic mushrooms, too little to trigger hallucinations or any sort of transcendental experience, but enough to, as its proponents suggest, “sharpen the mind.” Microdosers suggest that Psilocybin can induce creativity, calm anxiety, and even decrease the need for caffeine. However, it is worth noting that actual clinical research into microdosing is minimal.[45]
As was mentioned, a microdose can be anywhere between 5 to 10 percent of a normal dose. So, if a typical dose of mushrooms is 1.5 g, a microdose would be somewhere between 50 and 150 mg. Because of the low dosage, effects may be diminished on a full stomach. Most individuals suggest microdosing no more than twice a week and doing so well outside of work hours. For those who are interested in using these psychedelics as an addendum to therapy, experts recommend periodic breaks under supervision by professionals. It is also recommended to stay away from any kinds of stimulants like coffee, and to wait at least 3 to 4 hours to microdose if you have taken any prescription drugs. It is not safe or advisable to mix Psilocybin mushrooms with alcohol or other drugs.[46]
Side Effects, Safety & Toxicity
Part of the reason why researchers are so interested in Psilocybin’s therapeutic potential is because of its low toxicity relative to other hallucinogenic substances. However, it is possible to overdose on Psilocybin and develop toxicity symptoms, including hypertension, tachycardia, nausea, anxiety, vertigo, motor incoordination, and disorientation. In the best circumstances, these toxicity issues generally resolve between 4 to 12 hours after ingestion, and usually hospitalization is not required. Nevertheless, seeking medical attention is generally the best call if one has concerns about one’s reaction to magic mushroom ingestion.[47]
Furthermore, one must also be very cautious if one decides to purchase magic mushrooms. Aside from being illegal in most places, some have been known to sell store-bought mushrooms laced with PCP or LSD, which exacerbates the risk of a very bad reaction in the best case and fatal overdose in the worst.
A rare but serious potential side effect of taking Psilocybin in large doses is the possibility of developing Hallucinogen-Induced Persisting Perception Disorder, or HPPD, which causes individuals to have flashbacks of their psychedelic-induced hallucinations, causing severe distress in most patients.[48]
There are no published studies on the short- or long-term effects of using magic mushrooms during pregnancy, and therefore it is not advised for individuals to micro- or macro-dose Psilocybin while pregnant or breastfeeding.[49]
To sum, while there are many potential therapeutic benefits to taking Psilocybin mushrooms in small doses, using these hallucinogenic substances recreationally and in moderate- to high-doses carries a not-insignificant risk profile, even though Psilocybin is relatively low in toxicity compared to similar drugs.
Clinical Trials & Research Studies
According to ClinicalTrials.gov, there are a number of compelling studies to be on the lookout for all over the globe. For example, the Psychiatric Center Copenhagen at Rigshospitalet in Copenhagen is currently in the preliminary stages of designing a study evaluating Psilocybin’s efficacy as a treatment in patients with alcohol use disorders. Another promising study is currently recruiting at the University of California San Francisco and is exploring Psilocybin’s therapeutic potential in treating individuals suffering with depression and anxiety alongside Parkinson’s Disease. Also at the University of California San Francisco, a preliminary study is evaluating Psilocybin therapy for depression in Bipolar II. Several other studies – many of which are presently underway – are focused on Psilocybin’s effects on Major Depressive Disorder, including the Pacific Neuroscience Institute in Santa Monica, California, Yale University, Kadima Neuropsychiatry Institute in La Jolla, California, and Sheaf House Talaght Hospital in Dublin, Ireland. It appears that there will be particular attention devoted to the exploration of Psilocybin as an antidepressant medication, given its new status as a “breakthrough” drug with the FDA in recent years. Other studies of interest address Psilocybin’s potential role in the treatment of Body Dysmorphic Disorder, Anorexia Nervosa, and Obsessive Compulsive Disorder (OCD).[50]
Chemical Structure
Psilocybin is a tryptamine alkaloid under the genus Psilocybe, with hallucinogenic, anxiolytic, and psychoactive properties. In vivo, Psilocybin is dephosphorylated into the bioactive compound psilocin, which activates serotonin 2A (5-HT2A) receptors in the central nervous system.[51] Being lipid-soluble, psilocin crosses the blood-brain barrier to elicit its effects.[52]
Psilocybin and Psilocin differ in their chemical structure; specifically, Psilocybin has a phosphate group where Psilocin has a hydroxyl group. They are, however, both structural analogs of serotonin.[53] The similarities and differences in the chemical structures of these molecules can be visually observed in the image below.
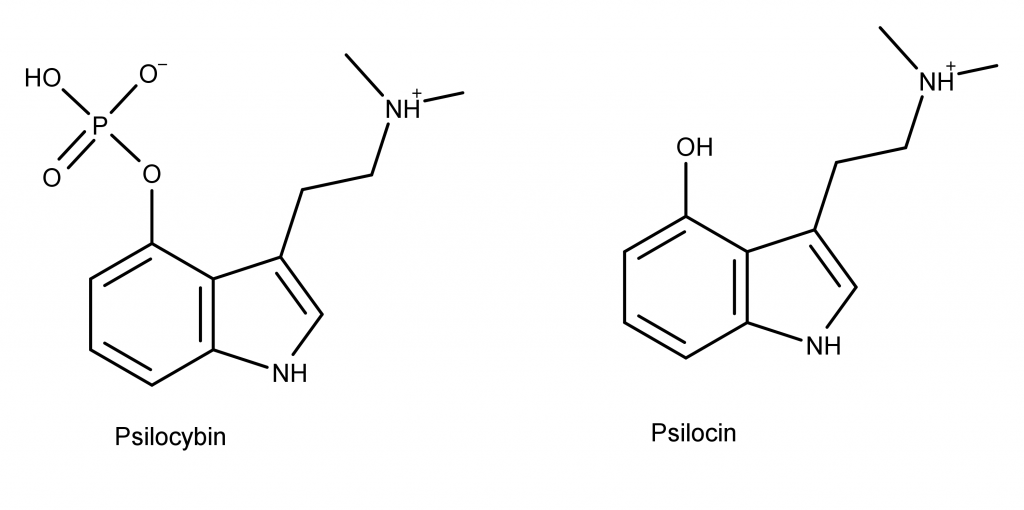
Best Ways to Take Psilocybin
One can ingest via Psilocybin by eating magic mushrooms directly, but consumers often report that the fungus itself doesn’t taste particularly good. Fortunately, there are other options besides eating the mushrooms whole. Some make Psilocybin tea by grinding the mushrooms into a fine powder and adding chopped-up ginger, honey, and/or a tea bag into the hot water. Mushroom capsules are another option; one simply needs empty capsules, a capsule machine, and a grinder.[54]
Legalization & Decriminalization
The movement to decriminalize Psilocybin began in earnest around the 2010s in the United States. Denver, Colorado was the first city to decriminalize the substance in May of 2019. Oakland and Santa Cruz, California followed in June 2019 and January 2020, respectively. No other cities followed suit for some time, until finally Washington, D.C. decriminalized Psilocybin in November 2020, followed shortly thereafter by Somerville and Cambridge, Massachusetts in January and February 2021, respectively.
However, this does not necessarily mean that Psilocybin is fully legal in all these cities. For example, in Denver, “decriminalization” really means that the city is not able to allocate any special resources to prosecute individuals over 18 for possession of Psilocybin. However, it is still illegal to sell and purchase Psilocybin. In Santa Cruz, the legalization of Psilocybin is still somewhat tenuous, meaning that adult possession and cultivation of Psilocybin is not illegal, but sale and purchase of the substance is, in fact, still illegal. There are still ongoing efforts to fully decriminalize Psilocybin throughout the United States. However, these petitions rarely garner enough signatures and support.
In 2020, Health Canada granted some exemptions to a number of health care professionals who wanted to possess and utilize mushrooms containing Psilocybin in a rather controversial move. Next, in a landmark decision in August of the same year, Health Canada approved four cancer patients’ request to legally use the drug for end-of-life palliative care.[55]
In the summer of 2020, almost 15,000 Canadians signed an online petition calling for the decriminalization of certain plants and fungi containing psychoactive properties, including Psilocybin. Backed by Decriminalize Nature Canada, an initiative of the Canadian Psychedelic Association, Petition e-2534 was presented to the House of Commons in September of 20202. However, pointing to existing legal mechanisms that allow access to controlled substances through certain exemptions, the government ultimately concluded that full decriminalization in Canada was not necessary.[56]
In most other parts of the world, the sale and purchase of Psilocybin remains illegal. However, there are a few exceptions, including The British Virgin Islands in the Caribbean, where it is legal to consume and possess Psilocybin but illegal to purchase and sell it. In Jamaica, similarly, magic mushrooms are sold quite openly, as there is no specific law that prohibits it. The situation is similar in Nepal. In Italy, it is legal to purchase, sell, and possess grow kits and Psilocybin spores for mushroom cultivation. In the Netherlands, it is possible to legally purchase Psilocybin in truffle form alone.[57]
Where to get Psilocybin?
There are over 180 different species of mushrooms containing Psilocybin that grow around the globe. Genera containing Psilocybin mushrooms include Copelandia, Gymnopilus, Inocybe, panaeolus, Pholiotina, Pluteus, and Psilocybe. The most common type of mushroom is Psilocybe cubensis. This type of mushroom is aesthetically distinctive because of its relatively large size and the fact that its cap widens with maturity. While different strains of Psilocybe cubensis can be found in the wild all over the world, the types that are grown indoors are generally more potent, as they are often bred for strength and grown in specific substrates that increase potency.
Another common type is Psilocybe semilanceata, or Liberty Caps, which is considered the most widespread naturally growing Psilocybin mushrooms in the world, and the third most potent. Psilocybe semilanceata was the first European native mushroom to be identified (as early as 1838) and formally recognized in scientific circles. This species is wildly popular and abundant, especially in England, but it is also common in fields in Germany, France, Finland, Iceland, Russia, Italy, Bulgaria, and Turkey. Some of these mushrooms have also been found on the West and East Coasts of North America, as well as Chile and New Zealand. Psilocybe semilanceata prefers rich and acidic soil, like grasslands, meadows, pastures, and lawns, especially those fertilized with cow or sheep manure.
One of the strongest magic mushroom strains is Psilocybe azurescens, or the Flying Saucer Mushroom. Also known as Blue Runners or Blue Angels, they are the most potent types of magic mushrooms that thrive in the wild. They are only found on the West Coast of the United States and prefer to live in sandy soils, such as near dunes and sea grasses. They have some of the highest percentages of Psilocybin (up to 1.78%), psilocin (0.38%), and baeocystin (0.35%). For this reason, there are potential side effects of temporary paralysis after ingesting high doses of this particular strain.
Next, there is the rare Psilocybe tampanensis, or Magic Truffles. These types of magic mushrooms are often sold at specialty shops and are commonly ingested on magic truffle retreats in the Netherlands. They are atypical to find in the wild but are popular for home cultivators. Consumers report that nausea can be more intense with this kind of mushroom, but nevertheless it remains a popular strain.
As was mentioned, there are over 180 different species of Psilocybin fungi, so the aforementioned only constitute a few of the more popular and recreationally ingested mushroom types.[58]
Growing vs Buying Psilocybin
The sale and purchase of Psilocybin mushrooms remains illegal in most countries, though it is decriminalized in some cities to a certain extent, as was previously discussed. For that reason, buying magic mushrooms can be tricky, risky, and ill-advised. Foraging for mushrooms in the wild also carries with it significant risks, as misidentifying a mushroom could be fatal.
Fortunately, growing magic mushrooms at home is relatively easy, though it does require some patience and significant attention to safety and hygiene. Probably the most challenging aspect is attaining a spore syringe from a reputable supplier; if the syringe is not properly designed, one could end up with contaminated or impotent spores, as the purpose of the item is to “sow” the spores into the substrate. A good mushroom grow kit will generally include a spore syringe, substrate, and grow bag; some even contain the mycelium itself. All equipment should be cleaned with rubbing, alcohol, and disinfectant, and handled with Latex gloves and a surgical mask. It generally takes 1 to 2 months to cultivate Psilocybin mushrooms indoors.[59]
Synthetic Psilocybin
As a result of the increased interest in Psilocybin therapy in recent years, researchers have been exploring the market’s demands through the development of synthetic Psilocybin. For example, COMPASS Pathways PLC, a pharmaceutical company based in the United Kingdom, developed a proprietary formulation of synthetic Psilocybin, COMP360, for use in research and clinical trials in 2021. They are currently conducting randomized controlled studies with patients suffering from mental health concerns, operating under the premise that COMP360 is a safer, more controlled alternative to natural psychoactive mushrooms. With this all being said, creating synthetic Psilocybin is expensive and very complex, so it may be quite some time before any products similar to COMP360 hit the market.[60]
Other companies that are currently developing synthetic Psilocybin options include Germany’s ATAI Lie Sciences and Calgary-based Psygen Labs.[61]
Interactions & Pairings
Psilocybin & Adderall
There has been no clinical research conducted into the interactions between Psilocybin and the drug Adderall, which is essentially a combination of the nervous system stimulants amphetamine and dextroamphetamine. However, in doing some research into anecdotal evidence, one often finds that Adderall and Psilocybin are contraindicated. Users have reported that the combination of the two substances is potentially dangerous, and likely to make the mushroom trip “paranoid and unpleasant.” Further, in sufficient quantities, combining mushrooms with an amphetamine like Adderall could result in serotonin syndrome, which causes agitation, confusion, delirium, is potentially fatal, sometimes causing renal failure and/or severe hypertension.[62]
Psilocybin & Cannabis
There is limited clinical research evaluating the combination of these two substances. However, the Internet is full of articles by individuals self-administering Psilocybin and marijuana or cannabis together. People often report that cannabis in particular “intensifies the trip,” particularly when doses of Psilocybin are relatively high. However, this intensification is not always positive. A 2019 literature review published by the Journal of Addictive Diseases noted a clinical presentation of Hallucinogen Persisting Perception Disorder (HPPD), a condition characterized by continuing hallucinations even off psychedelics, among subjects who had paired Psilocybin with additional substances, including cannabis. It was a small sample size of three individuals but should still serve as a word of caution for the user.[63]
Psilocybin & Alcohol
Psilocybin and alcohol are contraindicated. Combining these two substances can induce nausea and vomiting, faintness, hallucinations, paranoia, panic attacks, elevated anxiety, dehydration, and even seizures.[64]
Psilocybin & Lions Mane
Stacking Lion’s Mane with Psilocybin has earned some popularity in the microdosing community. Some are turning to what is commonly referred to as The Stamets’ Stack (named for the renowned mycologist Paul Stamets), which combines Lion’s Mane with niacin (vitamin B3) and Psilocybin. This stack emerges in part from Lion’s Mane’s reputation as “nature’s brain food,” as it stimulates Nerve Growth Factors (NGF) or induces neurogenesis. Resultant benefits include increased memory, concentration, and focus, better gut health, and the regeneration of auditory and visual neurons. At the level of this particular microdose, Psilocybin has a sub-perceptual effect, though it does have the potential to reduce anxiety and irritability and enhance cognitive functions. According to users, this stack is safe; however, the niacin component is not recommended for those who have liver diseases, stomach ulcers, very low blood pressure, renal difficulties, or who have ingested alcohol recently. With this all being said, there is no clinical evidence conducted on the efficacy of The Stamets’ Stack; evidence is anecdotal.[65]
Psilocybin & Lithium
There is strong evidence to indicate that Psilocybin is not safe to take alongside Lithium, which is a psychiatric mood stabilizer used to treat Major Depression and Bipolar Disorder. For example, in a study with the Johns Hopkins University School of Medicine, researchers found that 47% of patients who tried to combine Lithium plus classic psychedelics like LSD and Psilocybin reported incidents involving seizures. Further 39% of Lithium patients who used Psilocybin along with the medication reported that they required immediate medical attention. Researchers concluded that psychedelic use alongside Lithium poses a statistically significant seizure or medical emergency risk.[66]
Frequently Asked Questions (FAQ)
Can you overdose on Psilocybin?
It is extremely rare for individuals to overdose to the point of death from Psilocybin. However, it is indeed possible to overdose to the degree that one might experience severely unpleasant symptoms and even long-term psychological damage in the worst of cases. Symptoms of an overdose might include irritability or agitation, vomiting, stomach upset, severe anxiety, panic attacks, paranoia, and in severe cases, seizures, and long-term psychosis.[67]
Is Psilocybin Addictive?
Psilocybin is not considered to be a physiologically addictive drug. However, psychological dependence can develop and magic mushrooms are considered to have a high potential for abuse. In other words, people who are addicted to several drugs (poly-drug addicts) frequently abuse hallucinogens like magic mushrooms alongside their typical drug.[68]
What is Sex like on Psilocybin?
Psilocybin intensifies all the senses, including touch. This means that physical intimacy can potentially feel better than ever before. However, some anecdotal evidence indicates that the norms for what individuals typically enjoy during sex can change under the influence of Psilocybin. For example, an individual who likes a certain amount of pressure or aggressiveness during sex may become oversensitive and prefer less stimulation during intercourse.[69]
Want to know more? We have an entire article dedicated to Sex on Shrooms.
Does Psilocybin show on Drug Tests or Hair Follicle Tests?
Yes, a hair follicle test can detect the use of mushrooms from the last 90 days. However, mushrooms are unlikely to show up on a 5-panel test, which usually detects THC, cocaine, PCP, amphetamines, and opioids.[70]
Can you die from taking Psilocybin?
Magic mushrooms have very low toxicity, and death due to overdose is extremely rare. One survey in 2016 reported that, of roughly 12,000 users who took Psilocybin, only 0.2% recounted the need for emergency medical treatment.[71]
Is Psilocybin Approved by the FDA?
In 2019, the FDA granted Psilocybin the designation of a “breakthrough” therapy in the treatment of major depressive disorder. Researchers are currently exploring the substance as a therapeutic in a series of multi-phase clinical trials. However, it will likely be several years before these kinds of Psilocybin therapies actually hit the market.[72]
Can you have withdrawal from Psilocybin?
Yes, one can experience withdrawals from Psilocybin. Symptoms may include flashbacks to the trip, fatigue, insomnia, irritability, confusion, and memory loss.[73]
Is Psilocybin a stimulant?
Psilocybin mushrooms are considered to be hallucinogenic Schedule I drugs, not stimulants. Stimulants, commonly called “speed” or “uppers” arouse the central nervous system and include amphetamines, cocaine, ecstasy, and Ritalin, among other similar substances (including caffeine).[74]
References:
[1] Kargbo R.B. (2020) Psilocybin Therapeutic Research: The Present and Future Paradigm. ACS Medicinal Chemistry Letters, 11(4): 399-402.
[2] Ali A., Gordon L., Grant J., Lowe H., et al. (2021) The Therapeutic Potential of Psilocybin. Molecules, 26(10): 2948.
[3] Rootman J.M., Kryskow P., Harvey K. et al. (2021) Adults who microdose psychedelics report health related motivations and lower levels of anxiety and depression compared to non-microdosers. Scientific Reports 11, 22479.
[4] Goldberg S.B., Pace B.T., Nicholas C.R. et al. (2020) The experimental effects of Psilocybin on symptoms of anxiety and depression: A meta-analysis. Psychiatry Research 284, 112749.
[5] Ross S., Bossis A., Guss J. et al. (2016) Rapid and sustained symptom reduction following Psilocybin treatment for anxiety and depression in patients with life-threatening cancer: a randomized controlled trial. Psychopharmacology, 30(12): 1165-1180.
[6] Barnby J.M. & M.A. Mehta (03 July 2018) Psilocybin and Mental Health – Don’t Lose Control. Frontiers in Psychiatry.
[7] Carhart-Harris R.L., Bostridge M., Rucker J. et al. (2016) Psilocybin with psychological support for treatment-resistant depression: an open-label feasibility study. Psychiatry, 3(7): 619-627.
[8] Carhart-Harris R.L., Giribaldi B., Watts R. (2021) The trial of Psilocybin versus Escitalopram for depression. The New England Journal of Medicine, 384: 1402-1411.
[9] Hendricks P.S., Johnson M.W. & R.R. Griffiths (2015) Psilocybin, psychological distress, and suicidality. Psychopharmacology, 29(9): 1041-1043.
[10] Krediet E., Bostoen T., Breeksema J. et al. (2020) Reviewing the Potential of Psychedelics for the Treatment of PTSD. International Journal of Neuropsychopharmacology, 23(6): 385-400.
[11] Bird C.I., Modlin N.L. & J.H. Rucker (2021) Psilocybin and MDMA for the treatment of trauma-related psychopathology. International Review of Psychiatry, 33(3): 229-249.
[12] Schindler E.A.D., Sewell R.A., Gottschalk C.H. et al. (2021) Exploratory Controlled Study of the Migraine-Suppressing Effects of Psilocybin. Neurotherapeutics 18, 534-543.
[13] Lugo-Radillo A. & J.L. Cortes-Lopez (2020) Long-term Amelioration of OCD Symptoms in a Patient with Chronic Consumption of Psilocybin-containing Mushrooms. Journal of Psychoactive Drugs, 53(2): 146-148.
[14] Kelmendi B. (November 29 2017 – Present) Efficacy of Psilocybin in OCD: a Double-Blind, Placebo-Controlled Study. Identifier: NCT03356483.
[15] Carter O.L. & J.D. Pettigrew (2010) Psilocybin slows binocular rivalry switching through serotonin modulation. Journal of Vision
[16] Hendin H.M. & A.D. Penn (2021) An episode of mania following self-reported ingestion of Psilocybin mushrooms in a woman not previously diagnosed with Bipolar Disorder: A case report. Bipolar Disorders, 23(7): 733-735.
[17] Gard D.E., Pleet M.M. Bradley E.R. et al. (2021) Evaluating the Risk of Psilocybin for the Treatment of Bipolar Depression: A Systematic Review of Published Case Studies. Journal of Affective Disorders Reports, 6: 100240.
[18] Meldrum B.S. & R. Naquet (1971) Effects of psilocybin, dimethyltryptamine, mescaline and various allergic acid derivatives on the EEG and on photically induced epilepsy in the baboon (Papio papio). Electroencephalography and Clinical Neurophysiology, 31(6): 563-572.
[19] Johnson M.W., Garcia-Romeau A. & R.R. Griffiths (2016) Long-term follow-up of Psilocybin-facilitated smoking cessation. The American Journal of Drug and Alcohol Abuse, 43(1): 55-60.
[20] Beadle A. (12 October 2021) Can Psilocybin Help Smokers Quit? This Clinical Trial Aims to Find Out. Neuroscience News & Research.
[21] Diab H. & B. Malcolm. (2020) Persistent Tinnitus after Inhaled N,N-dimethyltryptamine (DMT). Journal of Psychoactive Drugs, 53(2): 140-145.
[22] Several authors (October 2016) Basically cured with Psilocybin [Online forum posts]. TinnitusTalk Support Forum.
[23] Vann Jones S.A. & A. O’Kelly (2020) Psychedelics as a Treatment for Alzheimer’s Disease Dementia. Frontiers in Synaptic Neuroscience, 12(34).
[24] Seltenrich N. (26 January 2021) Psychedelics Show Promise for Treating Dementia. Psychedelic Science Review.
[25] Barrett F.S., Krimmel S.R., Griffith R.R. et al. (2020) Psilocybin acutely alters the functional connectivity of the claustrum with brain networks that support perception, memory, and attention. Neuroimage, 218: 116980.
[26] Healy C.J. (2021) The acute effects of classic psychedelics on memory in humans. Psychopharmacology, 238(3): 639-653.
[27] Meinhardt M.W., Pfarr S., Fouquet G. et al. (2021) Psilocybin targets a common molecular mechanism for cognitive impairment and increased craving in alcoholism. Science Advances 7(47).
[28] Bogenschutz M.P., Forcehimes A.A., Pommy J.A. et al. (2015) Psilocybin-assisted treatment for alcohol dependence: A proof-of-concept study. Journal of Psychopharmacology, 29(3): 289-299.
[29] Mollinedo-Gajate I., Song C., Sintes-Rodriguez M., et al. (2020) Psilocybin rescues sociability deficits in an animal model of autism. bioRxiv.
[30] Naftulin J. (14 January 2021) Researchers believe ‘magic’ mushrooms have the potential to curb obesity. Insider.
[31] Hendricks P. (October 6 2021 – Present) Psilocybin-facilitated Treatment for Chronic Pain. Identifier: NCT05068791.
[32] Anson P. (21 July 2021) Can Psychedelics Be Used to Treat Fibromyalgia? Pain News Network.
[33] Author unknown (n.d.) Our Studies. TrPR Program. University of California San Francisco.
[34] Bullock G. (20 September 2019) Mixing Meditation and Magic Mushrooms? Mindful.
[35] Ellison K. (3 April 2021) A new treatment may halt cluster headaches. But some say psychedelic drugs are the real answer. The Washington Post.
[36] Sewell R.A., Halpern J.H. & H.G. Pope. (2006) Response of cluster headache to Psilocybin and LSD. Neurology, 66(12): 1920-1922.
[37] Madsen M.K., Fisher P.M., Burmester D. et al. (2019) Psychedelic effects of Psilocybin correlate with serotonin 2A receptor occupancy and plasma Psilocybin levels. Neuropsychopharmacology 44, 1328-1334.
[38] Dockrill P. (8 January 2018) Magic Mushrooms Do the Opposite of Anti-Depressants, But That May Be Why They Work. Science Alert.
[39] Hathaway B. (5 July 2021) Psychedelic spurs growth of neural connections lost in depression. YaleNews.
[40] Paul Stamets (n.d.) Neurogenesis confirmed in recent study
[41] Lee N. & B. Jones (27 April 2021) How magic shrooms affect your brain. Insider.
[42] Pollan M. (4 June 2018) What It’s Like to Trip on the Most Potent Magic Mushroom. The Atlantic.
[43] Woolfe S. (17 August 2021) 3 Things to Expect When Taking A Mushroom Trip. Healing Maps.
[44] Jikomes N. (n.d.) How to dose psychedelic mushrooms. Leafly.
[45] Begley S. (23 August 2018) ‘Microdosing’ is touted by ‘shroomers and Reddit users. Science is starting to test their claims – and finding some truth. Stat News.
[46] DiMatteo E. (23 July 2020) A beginner’s guide to microdosing. The Georgia Straight.
[47] Jo W.S., Hossain M.A. & S.C. Park (2014) Toxicological profile of poisonous, edible, and medicinal mushrooms. Mycobiology, 42(3): 215-220.
[48] Mitrokostas S. (24 January 2019) 10 potential risks of taking ‘magic’ mushrooms. Insider.
[49] Author unknown (28 October 2020) Can Pregnant Women Eat Mushrooms | Psychedelic Shrooms & Pregnancy? Magic Mushrooms 101.
[50] Clinical trials: Psilocybin (2021-Present) ClinicalTrials.gov.
[51] Author unknown (n.d.) Psilocybine. National Library of Medicine.
[52] Bauer B.E. (13 March 2019) The Pharmacology of Psilocybin and Psilocin. Psychedelic Science Review.
[53] Author unknown (n.d.) The Chemistry of Psilocybin. Psychedelic Science Review.
[54] Riggs M. (March 2021) How to Take Shrooms. Reason Magazine.
[55] Adlin B. (8 December 2020) Canada Will Let Health Care Professionals Legally Use Psychedelic Mushrooms, Health Minister Says. Marijuana Moment.
[56] Ball H. (1 November 2021) What is the future of the “Psychedelic Renaissance” in Canada? McGill Journal of Law and Health.
[57] Morski L.M. (1 February 2021) Where Can One Legally Take Magic Mushrooms? Way of Leaf.
[58] Janikian M. (6 April 2020) Types of Magic Mushrooms: 10 Shroom Strains You Should Know About. Double Blind Magazine.
[59] Morski L.M. (24 September 2020) How to Grow Magic Mushrooms [All You Need to Know]. Way of Leaf.
[60] Rozenbaum M. (1 October 2021) Depression and magic mushrooms: could synthetic Psilocybin cure untreatable depression? Understanding Animal Research.
[61] Author unknown (15 June 2021) Top 3 Psychedelic Companies Working With Synthetic Psilocybin. Microdose.
[62] Willis D. (2021) How does the prescription medication Adderall interact with recreational street drugs like magic mushrooms and marijuana? [Online forum posts]. Quora.
[63] Peters A. (25 November 2020) Combining cannabis with psychedelic mushrooms: Recipe for mind expansion or a bad trip? Leafly.
[64] Author unknown (14 October 2021) What are the Effects of Mixing Alcohol and Mushrooms? American Addiction Centers.
[65] Author unknown (n.d.) (Stacking Lion’s Mane). Microdosing Institute.
[66] Nayak S.M., Gukasyan N., Barrett F.S. et al. (2021) Classic Psychedelic Coadministration with Lithium, but Not Lamotrigine, is Associated with Seizures: An Analysis of Online Psychedelic Experience Reports. Pharmacopsychiatry, 54(5): 240-245.
[67] Author unknown (n.d.) Psychedelic Shrooms Overdose. Chapters Capistrano.
[68] Lewis T. (16 January 2020) Johns Hopkins Scientists Give Psychedelics the Serious Treatment. Scientific American.
[69] Ross M. (n.d.) Sex on Magic Mushrooms: Is It Safe? Infused Health.
[70] Carter A. (23 January 2020) Will Mushrooms Show Up On A Drug Test? Healthline.
[71] Wagener D. (22 May 2020) Can You Die From Taking Too Many Psychedelic Shrooms? Desert Hope Treatment Center.
[72] Feltman R. (26 November 2019) The FDA is fast-tracking a second Psilocybin drug to treat depression. Popular Science.
[73] Author unknown (n.d.) Psilocybin Mushroom Detox and Withdrawal. Rehab Spot.
[74] Author unknown (n.d.) Stimulants, Benzodiazepines, Mushrooms. Princeton University Health Services.


